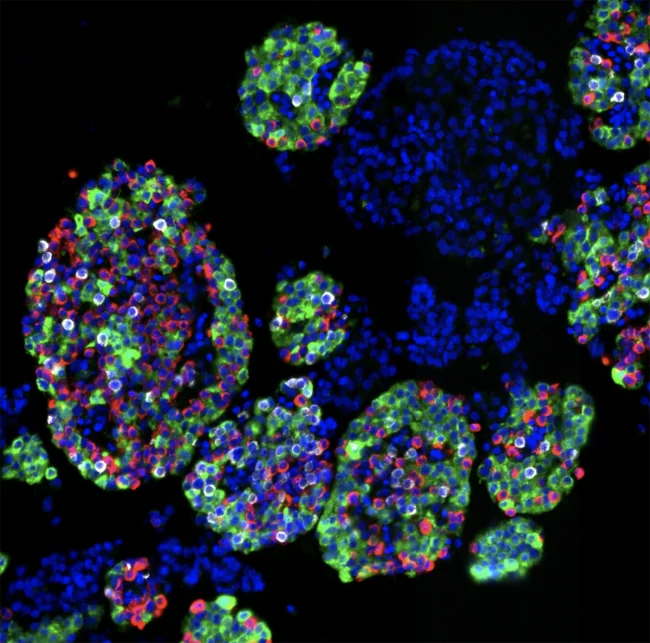
A National Institutes of Health (NIH)-funded study analyzing pancreatic islet cells from 299 organ donors has identified significant variation in the composition of hormone-producing cells that regulate blood sugar, shedding light on factors that may contribute to diabetes risk.
The research utilized islets collected through the NIH-supported Integrated Islet Distribution Program (IIDP) at City of Hope, California, which supplies the largest repository of human pancreatic islets for research. Scientists investigated differences among alpha, beta, and delta cells—each critical for controlling blood glucose through hormone secretion.
On average, islets consisted of 34% alpha cells (which produce glucagon to raise blood sugar), 58% beta cells (which produce insulin to lower blood sugar), and 8% delta cells (which regulate hormone secretion through somatostatin). However, considerable variability was observed in the proportions of alpha and beta cells across donors, with delta cell percentages also varying to a lesser extent.
Researchers linked these cellular differences to donor characteristics, including sex, race, ethnicity, and genetic factors such as predicted ancestry and diabetes risk profiles. For example, female-derived islets contained a higher proportion of alpha cells and fewer beta cells compared to males. Variations in beta cell percentages were also noted among different ancestry groups.
The study further demonstrated that islet cell composition strongly influences hormonal function: islets with more beta cells exhibited stronger insulin secretion, whereas those with higher alpha and delta cell counts tended to secrete less insulin. This suggests that the balance of cell types, rather than islet size or shape, plays a crucial role in glucose regulation.
“This level of characterization across so many donors has not been done in the past,” stated Albert J. Hwa, Ph.D., program director at NIH’s National Institute of Diabetes and Kidney Diseases (NIDDK). Co-lead author Carmella Evans-Molina, M.D., Ph.D., highlighted the diverse donor pool reflecting the U.S. population, vital for understanding population-wide differences.
Why it matters
The findings provide a detailed map of human islet cell variation linked to genetic and phenotypic diversity, offering new insights into how diabetes risk may be influenced by individual differences in pancreas biology. This dataset can serve as a resource for the diabetes research community to explore how genetic and environmental factors together affect disease development.
Background
Pancreatic islets contain specialized cells that secrete hormones crucial for blood sugar regulation. Dysfunction or altered proportions of these cells play a significant role in diabetes onset and progression. The IIDP supports research by providing high-quality human islets, enabling studies like this to investigate underlying mechanisms of diabetes at a cellular level.
The study, published in Nature Communications, was supported by NIH grants from the NIDDK and the National Institute of General Medical Sciences. The comprehensive analysis advances understanding of the biological diversity contributing to diabetes, a metabolic disease affecting millions in the U.S. and worldwide.
Sources
This article is based on reporting and publicly available information from the following source:
Read more Health & Public Health stories on Goka World News.